Today’s low-carb lesson, What is a calcium score and what do we do with the results?
I was fortunate to interview Ivor Cummins who has become a world expert on calcium scanning and some of the root causes of atherosclerosis.
Ivor Cummins has rapidly become one of the world’s experts on calcification scanning. He has recently presented at the British Association of Cardiovascular Prevention and Rehabilitation (BACPR) and also at the Irish National Institute of Preventative Cardiology (NIPC) annual conferences.
Ivor Cummins can be found through his website Fat Emporer CLICK HERE and the IDHA, Irish Heart Disease Awareness. CLICK HERE.
Are you ready to create the ultimate 12-month blueprint for reaching your health & weight loss goals this coming year?

Our free on-demand video training will walk you through how to make 2024 THE year you set health goals…and keep them.
What is a calcium scan?
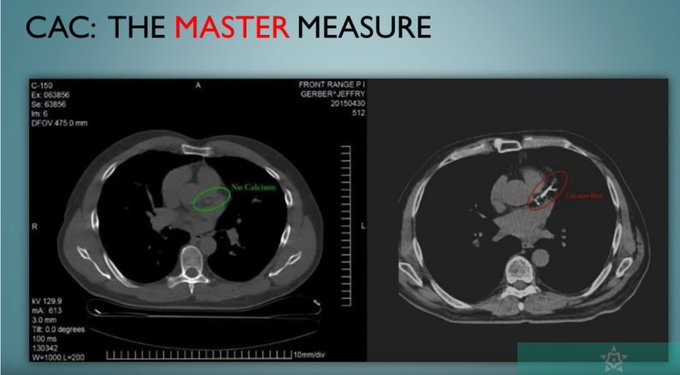
It’s a CT scan of the heart. It shows you directly what is actually happening rather than a risk factor of what may happen.
A calcium scan is quick, cheap and non-invasive.
Currently, there are a few options. You may get a CIMT carotid scan (a relatively poor risk predictor but it can track progression). You may have multiple blood factors measured which then is put into algorithms to determine your risk.
Or you may have a CT angiogram where they inject dye into you to get a clearer picture. If you have symptoms and high risk, this may be necessary but it may be too much for an asymptomatic middle/low-risk person
Because the heart moves so rapidly, for decades they could only take x-rays, but it was blurred. In the 1970’s they developed a high-speed electron beam, a super speed x-ray which could effectively take a rapid snapshot of the heart.
These clear images began to reveal calcium build-up in coronary arteries in some people, whilst some people had almost none. They also observed many patients had all the risk factors for heart disease, but with zero calcification.
The converse was also true. No risk factors but an incredibly high level of calcification.
What is a calcium score (and calcification)?
A calcium score shows the actual disease level, it doesn’t guess. It is a direct marker of atherosclerosis.
Calcification is the natural progression of arterial disease. As the plaques in your arteries burst open (like a pustule) they bring in calcium to stabilise them. The amount of soft plaque and dangerous plaque is directly correlated to the amount of calcium.
Someone with a very low level of calcium means they have very little of any type of plaque. And those with high calcification mean they have extensive plaque formation and soft plaque.
Seeing calcium in coronary arteries is the tip of the iceberg. It shows where plaques have been, where they are rupturing, and where there is calcium, soft plaque will be below.
Why do some people have no risk factors (yet have heart disease)?
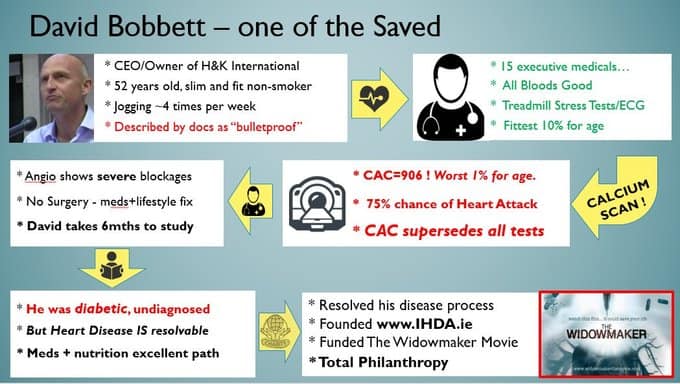
Many slim patients are often referred to as TOFI, thin outside fat inside. They appear to be healthy and slim but actually have fat surrounding their organs and be insulin resistant. They may also have extensive coronary artery disease. This is why it is so crucial to have a CAC scan.
President Clinton and some past astronauts, suddenly discovered they have extensive heart disease after undergoing a CAC scan.
These are men that you would think are at the peak of health, slim, have previously passed every single cardiovascular health test, stress test, and have been incredibly fit and active. Yet calcification wasn’t discovered until it was almost too late.
Often their blood markers appear OK because they are still consuming a high level of carbohydrates without realising the inflammatory change and damage it is doing to them.
Those who sit on the couch, smoke, and are overweight, will more often than not ring alarm bells with their doctors and they will get a lot of attention
Read more: Watch The Widowmaker Movie, Free
Who should have a CAC scan?
“It’s the middle-risk people”.
Low risk: If multiple blood markers are all good, and your algorithm risk score is below 5% risk of a heart attack in the next 10 years = very unlikely to have a high calcium result.
Middle risk: The majority of people now are middle risk. When these middle-risk people are scanned, 70% can be moved into either low-risk or high-risk category. So a CAC scan can determine whether you need aggressive treatment (if calcification has been confirmed) or de-prescribed (if it has been confirmed there are low or very low levels of calcification).
High risk: Who have multiple poor blood markers, they almost certainly have a problem. You don’t need a scan to know they are at very high risk and will have high levels of calcification.
What does a CAC score mean?
Image credits and references are below.
Who is suggested to have a CAC scan? Middle-aged, middle-risk people, men over 40-45, women over 50-55.
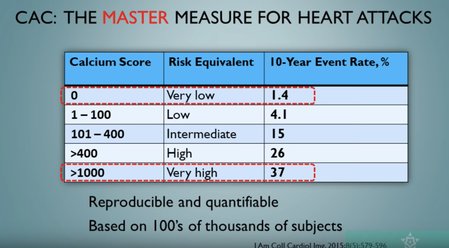
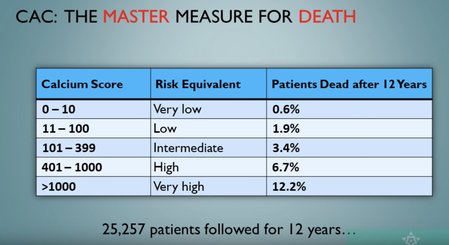
Calcium score: and risk of a heart attack in the next 10 years
- 0 = very low risk 1-1.5%
- 1-100 = moderate risk
- 100-400 = high risk
- 400+ = really high risk
- +1000 = 30% chance
Medications can stabilise the plaque especially in those with extensive and progressive disease. The latest studies indicate a statin may be required if a calcium score is over 100, below 100 a statin may have no benefit over 12 years. Medications may mitigate the symptoms but not the root cause.
Lifestyle changes
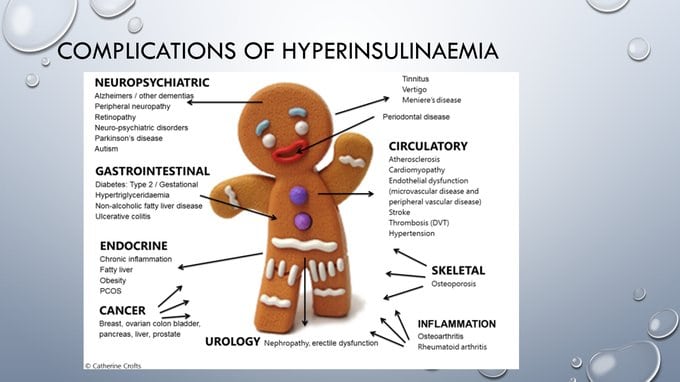
Photo credit: Dr. Catherine Crofts.
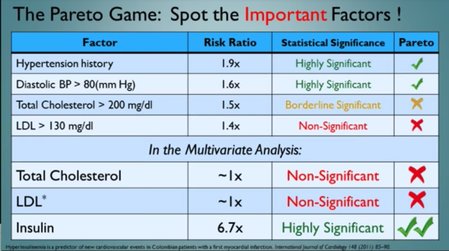
Knowing your calcium score allows you to take action, either way. The overwhelming biggest risk factor for developing an arterial disease, is diabetes, insulin resistance, and hyperinsulinemia. In the US, 65% of adults over 45 are either pre-diabetic or diabetic.
To get to the root cause of carbohydrate intolerance (diabetes), a low-carbohydrate diet and a low glycemic diet are indicated. Remove all sugars, starch, and junk food, because your body cannot handle them. Your body is intolerant to carbohydrates, especially in such large quantities.
LDL particles can be easily damaged by high blood sugars, high insulin and it damages their size and shape.
Read more: How To Start Low-Carb
Who benefits the most from statins?
People who have had a prior heart attack, those with a high calcium score, and those who have a genuinely high risk from the algorithms (low HDL, high LDL, high TG, high blood pressure, high HBA1C) may benefit from a statin.
NNT = number needed to treat. If you have a high calcium score, with lots of diseases, the NNT might be 20. So 20 people take statins for the next 10 years, 1 may get an appreciable benefit. But with a low calcium score, the NNT might be 120. 120 people have to take statins for the next 10 years, and 1 may get an appreciable benefit.
Top 3 Takeaways
- Middle risk, middle age, a calcium scan is recommended to confirm or reduce your risk.
- Fix the root cause. Medications (if indicated and benefit is clear), or lifestyle modifications. Aim to lower blood glucose, lower circulating insulin levels, lower HOMA IR, lower HBA1C.
- If you can stop your rate of progression of calcification your risk will plummet. If your calcium score only progresses by 5-15% each year (whereas the average person may increase by 25-35% each year), you are nearly as safe as someone with a low score.
3 Questions From Ditch The Carbs PRO Members
- What level of total cholesterol and LDL would you expect someone to begin a calcium scan or particle size count?
Do not look at LDL in isolation. Unless LDL is above 7.8mmol, it has no real use to predict heart attacks. Generally used as a treatment target. Instead, look at the risk MESA algorithms to calculate your risk. LDL particle count is not readily available and is still only a single measure. Better to look at Apo-B Apo-A1 ratio
- How often should you have a CAC scan if you find out your level is high, once a year is a long scary time to wait (to monitor progression).
Not to panic. Take all the right actions to address the root cause. If you have a high calcium score, then 18 months may be applicable. If you are low scoring, you could perhaps choose to wait 8-9 years. Calcium scores will show you the progression.
- What calcium score would you suggest a statin may be required?
The studies suggest a calcium score of over 100, you have a level of disease where a statin may be of benefit. If you are under 100, at a low level of risk and it is a conversation with your doctor. If you are paranoid about avoiding risk, you have a low level of disease but want to every single thing to avoid a possible heart attack you may decide to commence medication. Conversely, you may decide you have a low level of disease, are at low risk, the studies show you may not benefit and the side effects are too much to risk-taking medication, instead, fixing the root causes is a better option. But this must be an informed decision that you are happy and confident to make and are at peace with whatever you decide.
Conclusion
We make life decisions on a daily basis. We take risks when we drive. We take risks running across the road. Only you can decide what risks you take.
Only YOU can decide what risks to take in YOUR situation.
You have to be your own health advocate.
References:
- Avoiding and resolving modern chronic disease
- Progression of Coronary Artery Calcium and Risk of First Myocardial Infarction in Patients Receiving Cholesterol-Lowering Therapy
- Coronary Artery Calcium and Multisite Atherosclerosis: Role in Risk Refinement.
- Dr Agatston – Coronary Calcification to determine Heart Attack Risk
- Studies Suggest Coronary Calcium Score Indicates Long-Term Heart Health
- A zero coronary artery calcium score in patients with stable chest pain is associated with a good prognosis, despite risk of non-calcified plaques
- Dr. William David, Cardiologist – What Is Plaque – and how to Measure It?
- Dr Budoff, Professor of Medicine, UCLA School of Medicine
Image Credits: Ivor Cummins.
- Hyperinsulinemia is a predictor of new cardiovascular events in Colombian patients with a first myocardial infarction
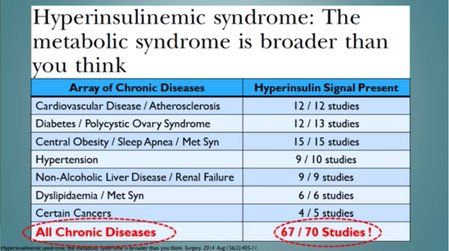
- Hyperinsulinemic syndrome: The metabolic syndrome is broader than you think
- Coronary Artery Calcium Scanning: Past, Present, and Future. JACC: Cardiovascular Imaging Volume 8, Issue 5, May 2015, Pages 579-596
Get our FREE guide to finally fix your metabolism!
Losing weight & getting healthy is never easy, but lately you might feel like it’s suddenly become impossible.
Our Flip the Switch guide will help you clearly understand what’s been going on, as well as exactly what you can do to get your metabolism working again so that you can look and feel your best—it’s easier and more simple than you think!










Why lowering carbs causes LDL to go up?